
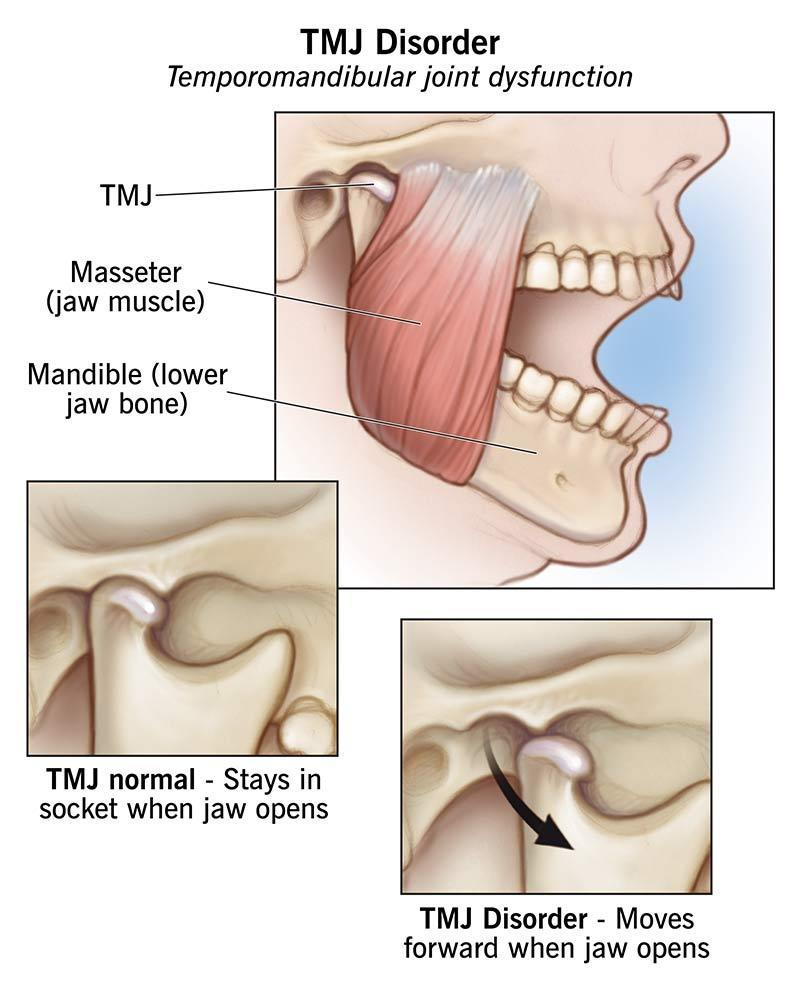
 (TMJ Disorders: Symptoms, Causes & Treatment) Normal vs. dysfunctional TMJ: The disc stays in place in a healthy joint (left), but may slip forward in TMJ disorder (right), causing pain or jaw locking. As dental professionals, we often encounter patients with jaw pain, clicking joints, or difficulty chewing. These issues may point to temporomandibular joint disorders (TMD) – a group of conditions affecting the jaw joints and chewing muscles. TMD is the most common non-odontogenic orofacial pain condition ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ), estimated to affect ~5–12% of adults (predominantly women 20–40 years old) (TMJ Disorders: Symptoms, Causes & Treatment). Early recognition and management are critical: timely intervention can relieve symptoms, prevent chronic joint damage, and improve quality of life ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ). Below is a comprehensive overview of TMD symptoms, signs, risk factors, diagnosis, and treatment options – and the pivotal role we play in early diagnosis and interdisciplinary care.
(TMJ Disorders: Symptoms, Causes & Treatment) Normal vs. dysfunctional TMJ: The disc stays in place in a healthy joint (left), but may slip forward in TMJ disorder (right), causing pain or jaw locking. As dental professionals, we often encounter patients with jaw pain, clicking joints, or difficulty chewing. These issues may point to temporomandibular joint disorders (TMD) – a group of conditions affecting the jaw joints and chewing muscles. TMD is the most common non-odontogenic orofacial pain condition ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ), estimated to affect ~5–12% of adults (predominantly women 20–40 years old) (TMJ Disorders: Symptoms, Causes & Treatment). Early recognition and management are critical: timely intervention can relieve symptoms, prevent chronic joint damage, and improve quality of life ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ). Below is a comprehensive overview of TMD symptoms, signs, risk factors, diagnosis, and treatment options – and the pivotal role we play in early diagnosis and interdisciplinary care.
Symptoms & Signs
Common symptoms: Patients with TMD may present with one or more of the following:
Jaw and facial pain: Persistent pain in the TMJ area or chewing muscles, often radiating to the face, neck, or temples (TMJ Disorders: Symptoms, Causes & Treatment) (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).
Limited jaw movement or locking: Difficulty or pain on opening the mouth wide, jaw “locking” open or closed, or stiffness in jaw movement (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).
Joint sounds: Clicking, popping, or grating sounds in the TMJ during opening/closing (especially if accompanied by pain) (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).
Headaches or ear symptoms: Tension-type headaches, earaches, a feeling of fullness in the ears, tinnitus (ringing in ears), or even dizziness not explained by ear pathology (TMJ Disorders: Symptoms, Causes & Treatment) (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).
Chewing difficulty: Discomfort or fatigue while chewing, or a sensation that the bite is “off” or teeth don’t fit together properly (TMJ Disorders: Symptoms, Causes & Treatment).
Note: Joint sounds (clicking/popping) without pain or dysfunction are common and usually do not require treatment (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). It’s important to distinguish benign joint noise from true TMD that needs intervention.
Clinical signs: On examination, a patient with TMD often exhibits:
Muscle and joint tenderness: Palpation of the masseter, temporalis, or TMJ elicits pain or soreness (TMJ Disorders: Symptoms, Causes & Treatment). Muscles of mastication may feel tight or enlarged from overuse (bruxism).
Reduced or uneven jaw motion: Limited mouth opening (e.g. <40 mm) or deviation of the jaw to one side upon opening/closing, indicating joint dysfunction or disc displacement (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).
Audible/palpable clicks or crepitus: The clinician may feel or hear clicking in the joint during movement (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). A coarse grinding noise (crepitus) could suggest degenerative changes.
Dental wear or occlusal changes: Excessive tooth wear, flat facets, or cracked teeth can signal chronic grinding/clenching (a contributing factor to TMD). Some patients also develop a change in occlusion as muscles spasm or disks displace.
Risk Factors
Understanding predispositions can help identify who is at risk for TMD. Key risk factors include:
Demographics: Female sex (TMD is about 2× more common in women) and age 20–40 are associated with higher prevalence (TMJ Disorders: Symptoms, Causes & Treatment) – possibly due to hormonal factors and stress during these years.
Bruxism (teeth grinding/clenching): Chronic grinding or clenching, especially during sleep or stress, places excessive load on the TMJ and muscles (TMJ Disorders: Symptoms, Causes & Treatment). This microtrauma is a leading contributor to TMJ pain and disc derangements.
Jaw trauma or injury: A history of jaw injury (e.g. impacts, whiplash, or jaw fractures) can damage joint structures or alter the bite, precipitating TMD (TMJ Disorders: Symptoms, Causes & Treatment). Even dental trauma or extended mouth opening (e.g. long procedures) might trigger symptoms in susceptible patients.
Arthritis: Osteoarthritis or rheumatoid arthritis affecting the TMJ can cause degeneration of the joint surfaces and inflammation (TMJ Disorders: Symptoms, Causes & Treatment). Patients with systemic arthritis may report TMJ pain, crepitus, or stiffness.
Chronic stress & muscle tension: Psychological stress is strongly linked to TMD (TMJ Disorders: Symptoms, Causes & Treatment). Stress can lead to increased jaw clenching, muscle hyperactivity, and heightened pain perception. Many TMD patients have anxiety, depression, or other chronic pain conditions as comorbidities.
Parafunctional habits & posture: Behaviors like frequent gum chewing, nail biting, pencil chewing, or holding tension in the jaw worsen TMD strain (TMJ Disorders: Symptoms, Causes & Treatment). Poor posture (forward head posture) can alter mandibular position and contribute to jaw muscle fatigue (TMJ Disorders: Symptoms, Causes & Treatment).
Joint hypermobility or connective tissue disorders: Patients with ligament laxity or disorders like Ehlers-Danlos syndrome have higher risk of TMJ instability and disc displacement (Ehlers-Danlos Syndromes - The TMJ Association). Generalized joint hypermobility can lead to recurrent subluxation of the jaw and associated pain.
Patients with one or more of these factors should be monitored closely for TMD symptoms. For example, a young adult woman with a stressful job and signs of bruxism is at heightened risk – proactive evaluation can catch TMD early.
Diagnosis
Diagnosing TMD can be challenging, as there is no single definitive test (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research) and symptoms overlap with other conditions. A systematic approach includes:
Thorough history: Document the patient’s symptoms (onset, duration, triggers, and alleviating factors) (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Ask about jaw injuries, dental treatments, oral habits, daytime or sleep bruxism, and associated symptoms like headaches or ear pain. Screen for related conditions (e.g. fibromyalgia, chronic headache) which commonly coexist ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ).
Clinical examination: Palpate the TMJs and masticatory muscles for tenderness, and evaluate jaw range of motion (TMJ Disorders: Symptoms, Causes & Treatment). Note any noise or deviations on movement. Assess dental wear facets, and check if any mandibular movements provoke pain. A standard exam includes listening to and feeling the jaw joints during opening/closing, and measuring interincisal opening (TMJ Disorders: Symptoms, Causes & Treatment).
Diagnostic imaging: Imaging is used to confirm joint alterations or rule out other pathologies. A panoramic X-ray can screen for gross bony changes or other jaw issues. CT scans provide detailed bony anatomy of the TMJ (e.g. condylar erosion or osteophytes) (TMJ Disorders: Symptoms, Causes & Treatment). MRI is the gold standard for visualizing soft tissues – it can show disc displacement or inflammation in the joint (TMJ disorders - Diagnosis and treatment - Mayo Clinic) (TMJ disorders - Diagnosis and treatment - Mayo Clinic). In complex cases, TMJ arthroscopy allows direct inspection of the joint and can aid in both diagnosis and treatment (TMJ disorders - Diagnosis and treatment - Mayo Clinic). Always consider differential diagnoses (toothache, sinus issues, otologic or neurologic causes) and use imaging or referrals to rule those out (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).
Diagnostic criteria: For consistency, practitioners can utilize the Diagnostic Criteria for TMD (DC/TMD), an evidence-based classification of the most common TMD conditions ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ). This helps classify the disorder (e.g. myofascial pain, disc displacement with reduction, arthralgia, etc.) and guides targeted treatment. In practice, a preliminary diagnosis (such as myofascial TMD vs. intra-articular TMD) can often be made clinically and refined with imaging if needed.
Who needs treatment? Essentially, any patient with persistent TMD symptoms (pain, functional limitation, or progressive change) should receive appropriate management. Mild cases may fluctuate, but if pain or locking interferes with quality of life, diagnostic workup and treatment are indicated. (By contrast, a patient with only occasional jaw clicks without pain likely just needs observation and habit counseling, not active treatment (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).)
Treatment Options
Management of TMD is typically conservative and tailored to severity. Because many TMD cases are self-limiting or improve with simple care, the first-line treatments are non-surgical and reversible (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). An interdisciplinary, stepwise approach is often most effective. Common treatment modalities include:
Self-care & habit modification: Begin with patient education and simple lifestyle changes. Advise a soft diet (avoiding hard or chewy foods), smaller bites, and rest for the jaw (TMJ disorders - Diagnosis and treatment - Mayo Clinic). Apply warm compresses or ice to the jaw (heat for muscle pain, ice for acute inflammation) to ease discomfort (TMJ disorders - Diagnosis and treatment - Mayo Clinic). Gentle jaw stretching and relaxation exercises (often taught by a dentist or physical therapist) help maintain mobility (TMJ disorders - Diagnosis and treatment - Mayo Clinic). Patients should be coached to avoid harmful habits – no gum chewing, pencil biting, jaw clenching, or leaning on the chin (TMJ disorders - Diagnosis and treatment - Mayo Clinic) (TMJ Disorders: Symptoms, Causes & Treatment). Improving posture and reducing overall stress (through techniques like meditation or mindfulness) also support recovery (TMJ Disorders: Symptoms, Causes & Treatment) (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). These self-management strategies can significantly reduce load on the TMJ and often alleviate mild TMD symptoms.
Medications: Pharmacological support is used to control pain and inflammation, especially in acute phases. Start with NSAIDs or analgesics (e.g. ibuprofen, naproxen) to reduce joint and muscle inflammation (TMJ Disorders: Symptoms, Causes & Treatment). For muscle spasm, short-term muscle relaxants (e.g. cyclobenzaprine) can be helpful (TMJ Disorders: Symptoms, Causes & Treatment). Low-dose tricyclic antidepressants (e.g. amitriptyline or nortriptyline) at night can help break chronic pain cycles, improve sleep, and even reduce bruxism intensity (TMJ disorders - Diagnosis and treatment - Mayo Clinic). In some cases, benzodiazepines or anxiolytics are prescribed short-term to relieve severe muscle tension, especially when stress is a big factor (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). (Always use caution with medications – consider referral for chronic pain management if opioids or long-term meds are needed (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).)
Oral appliances (splints): Stabilization splints or night guards are a cornerstone conservative therapy. A custom occlusal splint worn at night (or during stressful daytime hours) can reduce clenching/grinding forces and protect the teeth (TMJ Disorders: Symptoms, Causes & Treatment). Splints also help by slightly repositioning the jaw to a more relaxed muscular position, which may alleviate joint loading. Evidence on splint efficacy is mixed, but many patients report symptom relief with consistent use (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Important: the appliance should be reversible (e.g. a flat-plane night guard); avoid any device intended to permanently alter the bite. Monitor the patient – if a splint increases pain or causes new issues, discontinue or adjust it (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).
Physical therapy: Collaboration with a physical therapist (or trained dental specialist) can greatly benefit TMD patients. Jaw exercises improve range of motion and reduce pain – for example, gentle stretching of the jaw opening, lateral movements, and resisted closing/opening exercises to strengthen weak muscles (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Manual therapy techniques can release trigger points in the jaw and neck muscles, improving function (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Modalities like ultrasound therapy, low-level laser, or TENS (transcutaneous electrical nerve stimulation) may provide additional pain relief and muscle relaxation for some patients (TMJ Disorders: Symptoms, Causes & Treatment) (TMJ disorders - Diagnosis and treatment - Mayo Clinic). A PT can also work on posture correction and teach relaxation exercises for the neck and jaw. Studies consistently show combining splint therapy with physiotherapy yields better pain reduction than single-modality treatment ( Effects of an Interdisciplinary Approach in the Management of Temporomandibular Disorders: A Scoping Review - PMC ) ( Effects of an Interdisciplinary Approach in the Management of Temporomandibular Disorders: A Scoping Review - PMC ).
Behavioral therapy and stress management: Given the psychosocial component of many TMDs, addressing the mental health and behavioral aspects is important. Cognitive-behavioral therapy (CBT) with a pain psychologist can help patients manage stress, change oral habits, and cope with chronic pain (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Techniques like biofeedback (to become aware of and release jaw tension) and relaxation training can reduce parafunctional muscle activity (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Even simple mindfulness practices and good sleep hygiene may improve TMD symptoms by reducing overall stress on the jaw system. Encourage patients to recognize triggers (e.g. clenching during work stress) and develop healthier responses.
Injections and minimally invasive procedures: When conservative measures aren’t sufficient, targeted interventions can be considered. Trigger-point injections of a local anesthetic or corticosteroid into painful masticatory muscles can provide relief in myofascial TMD (TMJ Disorders: Symptoms, Causes & Treatment). Intra-articular corticosteroid injections into the TMJ joint can reduce inflammation in cases of acute arthritis or severe synovitis. Another option in select cases is Botulinum toxin (Botox) injections into overactive jaw muscles, which may ease chronic clenching and muscle pain (TMJ Disorders: Symptoms, Causes & Treatment). (Note: Botox for TMD is off-label and evidence is still limited (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research), but some patients with refractory muscle pain do benefit.) For patients with painful clicking or intermittent locking due to disc displacement, a simple arthrocentesis can be performed: flushing the joint through needles to wash out inflammatory byproducts and improve movement (TMJ disorders - Diagnosis and treatment - Mayo Clinic). Arthrocentesis is minimally invasive and can alleviate pain and improve mouth opening in cases with displaced discs (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research), though results may be temporary.
Surgical interventions (last resort): Surgery is reserved for severe TMD cases where structural joint damage is confirmed and all conservative treatments have failed. Options include TMJ arthroscopy (using a thin scope and instruments inserted via a small incision) to remove adhesions or reposition the disc, and open-joint surgery for major repairs (TMJ Disorders: Symptoms, Causes & Treatment). Arthroscopic surgery is less invasive and can moderately improve pain and function by smoothing the joint or freeing a stuck disc (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Open-joint procedures (e.g. disc repositioning, condylar reshaping, or total joint replacement) are rare and only indicated for extreme cases like tumors, ankylosis, or severe osteoarthritis with joint destruction (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research) (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). It’s vital to set patient expectations: surgical outcomes are variable, and surgery permanently alters the joint (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Always exhaust non-surgical options first – refer to an oral and maxillofacial surgeon or TMJ specialist if considering invasive measures, and ensure the patient understands the risks vs. benefits (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research) (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research).
Clinical tip: Experts strongly recommend avoiding irreversible treatments (like grinding down teeth or extensive orthodontic adjustments solely to “fix” TMD) unless absolutely necessary (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Malocclusion alone is rarely the primary cause of TMD, and permanently altering the bite can even worsen the condition (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research) (TMD (Temporomandibular Disorders) Causes, Symptoms, Diagnosis, Treatment | National Institute of Dental and Craniofacial Research). Therefore, reversible and conservative therapies are preferred as first-line approaches in TMD management.
Early Diagnosis & Collaborative Care
Early diagnosis is key. Identifying TMD in its early stages allows us to manage it with simpler, conservative treatments before chronic pain or joint degeneration set in. Many patients dismiss early signs like occasional jaw soreness or clicking – as clinicians, we should ask about these symptoms during routine exams. Prompt care can alleviate symptoms and prevent complications, improving the patient’s long-term outlook (Importance: Early Diagnosis and Treatment for TMJ Disorders) ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ). Research indicates that supporting early diagnosis and treatment of TMD leads to better prognosis, higher quality of life, and even reduced healthcare costs ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ). Encourage patients to report jaw pain or dysfunction sooner rather than later.
Interdisciplinary collaboration is often what leads to the best outcomes. TMD has a multifactorial, biopsychosocial nature ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ) – so management frequently requires a team effort. The combined skills of dentists, physiotherapists, pain specialists, and sometimes psychologists or ENT specialists are needed to address all aspects of the disorder ( Effects of an Interdisciplinary Approach in the Management of Temporomandibular Disorders: A Scoping Review - PMC ). For example, a dentist might provide an occlusal splint and adjust any dental contributors, a physical therapist can handle the musculoskeletal rehab, and a psychologist can assist with stress management or chronic pain coping. Regular communication among providers ensures consistent messages to the patient and a unified treatment plan.
The dental professional’s role is central in TMD care. We are often the first to evaluate the patient’s orofacial complaints and can coordinate multidisciplinary treatment. Key responsibilities include:
Screening and early identification: Incorporate TMD screening into dental exams – listen for joint sounds, ask about jaw pain, check range of motion. Early flags like significant tooth wear or patient reports of morning jaw pain should prompt a closer look.
Patient education: Educate patients on the link between their symptoms and possible habits or stress. Advise on home care (jaw rest, diet modifications, hot/cold therapy) and counsel them to avoid aggravating habits (TMJ Disorders: Symptoms, Causes & Treatment). Empowering patients with knowledge about TMD goes a long way in management.
Initial management: Dentists can initiate first-line treatments such as fabricating a custom night guard, prescribing anti-inflammatories, or teaching stretching exercises. These interventions can provide relief while further evaluations are underway. Monitor progress closely and adjust the plan as needed.
Referral and coordination: Know when to involve specialists. Refer to an orofacial pain specialist or oral surgeon if the diagnosis is uncertain or if advanced therapies (e.g. joint injections, surgery) are considered. Similarly, refer to physical therapy for muscle rehab or to behavioral health for pain management support. Coordinate care by sharing findings and treatment goals with the team – an aligned, interdisciplinary approach prevents fragmented care.
By staying vigilant for TMD and working collaboratively, dental professionals can significantly improve patient outcomes. Early, conservative intervention often prevents the progression to chronic, debilitating TMD. Meanwhile, an informed, team-based approach ensures all contributing factors – from occlusion to posture to anxiety – are addressed. In summary, patients who need TMJ treatment are those with persistent pain or jaw dysfunction, and they rely on us to recognize the signs early. Through education, early diagnosis, and interdisciplinary management, we can help our patients find relief from TMD and protect their long-term oral and joint health.
References: TMD is a complex topic, and ongoing research continues to refine best practices. Dental professionals are encouraged to stay updated with current guidelines and evidence-based recommendations for TMJ disorders ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ) ( Temporomandibular disorders: a review of current concepts in aetiology, diagnosis and management - PMC ). Early detection and a holistic treatment strategy are our best tools to manage this common yet often misunderstood condition. Together with our medical and therapy colleagues, we can ensure those who need TMJ treatment receive comprehensive, effective care.
